Colorectal
Dr Penelope De Lacavalerie specialises in the diagnosis and treatment of conditions in the lower intestine, rectum and anus. Utilising the latest in minimally-invasive surgical techniques, including the da Vinci X1 (R) System, Dr De Lacavalerie delivers leading comprehensive care focused on the best outcomes for her patients.
Colorectal
Dr Penelope De Lacavalerie specialises in the diagnosis and treatment of conditions in the lower intestine, rectum and anus. Utilising the latest in minimally-invasive surgical techniques, including the da Vinci X1 (R) System, Dr De Lacavalerie delivers leading comprehensive care focused on the best outcomes for her patients.
CONDITIONS AND PROCEDURES
BENIGN BOWEL SURGERY
INFLAMMATORY BOWEL DISEASE (IBD)
ENDORECTAL ULTRASOUND
For more information, download the brochure below.
ANAL MANOMETRY
For more information, download the brochure below.
SACRAL NERVE MODULATION

InterStim® – Treatment for Faecal Incontinence
Incontinence problems affects millions of Australians. If you’re one of them, you know how these conditions, like over-active bladder (OAB), faecal incontinence (involuntary loss of stool), and urinary retention can interrupt your life.
You may have tried changing your diet. Or Kegal exercises, physical therapy and biofeedback. Or medications with unpleasant side effects. But the results just aren’t what you hoped.
Communication between your brain and bowel is critical. That’s why conventional treatments may not produce the results you want- they don’t target the miscommunication between your bowel and brain.

Unlike conventional treatments, Medtronic Bladder and Bowel Control Therapies delivered by the InterStim system uses gentle nerve stimulation to correct the bladder/bowel-brain communication pathway and restore bladder and bowel function.
Medtronic Bladder and Bowel Control Therapy delivered by the InterStim system restore bladder and bowel function by gently stimulating the sacral nerves. It’s sometimes called sacral neuromodulation (SNM). With this therapy, you may experience fewer trips to the bathroom, fewer accidents and more confidence as you get back to the activities you enjoy.
Unlike conventional treatments, Medtronic Bladder and Bowel Control Therapies delivered by the InterStim system uses gentle nerve stimulation to correct the bladder/bowel-brain communication pathway and restore bladder and bowel function.
Medtronic Bladder and Bowel Control Therapy delivered by the InterStim system restore bladder and bowel function by gently stimulating the sacral nerves. It’s sometimes called sacral neuromodulation (SNM). With this therapy, you may experience fewer trips to the bathroom, fewer accidents and more confidence as you get back to the activities you enjoy.
InterStim is safe and minimally invasive. It’s been helping people improve their quality of life for more than 20 years
- 84% satisfaction among those who use it
- Greater improvements in quality of life compared to medications
- 89% of people achieve success at 5 years with InterStim therapy
- 36% of people achieve complete continence at 5 years with In InterStim therapy
Unlike other bladder and bowel control therapies, InterStim is the only therapy that allows you to try it first. It’s called an evaluation- like a test run, not a long-term commitment.
Here’s how it works
- The simple evaluation starts as day procedure
- A lead (thin wire) is placed in your upper buttock along the nerves that control your bladder
- The lead attaches to a small external device worn discreetly under your clothes
- Stop, start or adjust the therapy with a Samsung controller
- Go about most of your normal activities for 7 days
- Track your symptoms in a diary to see if they improve
After the end of your trial, talk with our team about the results. Did it feel successful? Did you see symptom improvement? Together, we will decide if the long-term therapy is the right choice. If it is, we can replace the external device with an implantable device called a neurostimulator during a short, out-patient procedure.

What is InterStim™ II?
The recharge-free InterStim™ II system gives patients freedom from a recharging routine, the hassle of recharging components, and a reminder they have a disease. InterStim™ II is simple, convenient, low maintenance. InterStim II now allows full-body 1.5 and 3 Tesla MRI conditional scans with SureScanTM MRI technology.

What is InterStim™ Micro?
The TGA recently approved the InterStim™ Micro neurostimulator, the market’s smallest and fastest rechargeable device to deliver sacral neuromodulation (SNM) therapy. It offers a smaller size compared to InterStim II and a longer battery life. InterStim Micro also allows full-body 1.5 and 3 Tesla MRI conditional scans with SureScanTM MRI technology.

What are the benefits of the new InterStim™ systems for patients with OAB or FI?
The recharge-free InterStim II system is simple and convenient with lower maintenance and time commitments. This specific system gives patients the freedom from a recharging routine, the hassle of recharging components, and a reminder they have a disease.
The InterStim Micro rechargeable system is the smallest device on the market with the fastest rechargeability and is stronger than other manufacturers’ batteries. It features proprietary Overdrive™ battery technology — a battery with virtually no loss in capacity over time.[i] The new battery technology allows patients to choose how and when they want to charge their device — from as often as once a week, or as infrequent as once per month, depending on the patient’s preference and device settings. There is no battery fade at 15 years* and patients can restart their therapy after extended breaks in time.
Visit https://www.medtronic.com/au-en/patients/treatments-therapies/bowel-control/considering-therapy.html to learn more.
FAQs
A: This therapy targets the nerves that control your bladder and bowel to help it function normally again.
A: Medtronic Bladder and Bowel Control Therapy delivered by the InterStim™ system restores bladder and bowel function by gently stimulating the sacral nerves.
A: It’s thought that bladder and bowel control problems are caused by miscommunication between the brain and the sacral nerves, which control the bladder and bowel and muscles involved in urination.
A: With this therapy, you may experience fewer trips to the bathroom, fewer accidents, and more confidence as you get back to the activities you enjoy.
A: Implanting an InterStim system has risks similar to any surgical procedure, including swelling, bruising, bleeding, and infection. Talk with your doctor about ways to minimize these risks.
A: It is the only advanced therapy for OAB that is clinically superior to oral medication. And it’s the only therapy that lets you try it first during an evaluation.
A: This therapy significantly reduced symptoms of OAB and non-obstructive urinary retention in people treated for 5 years. Your experience may be different.
A: No. It can be effective, but it’s not a cure. If the neurostimulator is turned off or removed, symptoms can return.
A: Most people describe it as a slight tingling, or fluttering sensation in the pelvic area. It should not be painful. Stimulation settings can be adjusted, and sensations will vary from person to person.
A: Getting a full-body MRI scan may be possible under specific conditions. For more information, talk with your doctor.
A: Medicare and most private insurance companies cover this therapy. Talk with our team to learn more about your insurance coverage.
A: It is an TGA-approved therapy doctors have used to treat bladder and bowel control problems for nearly 20 years. More than 325,000 people have received this therapy.
PELVIC FLOOR EXERCISES
For more information, download the brochure below.
FAECAL INCONTINENCE
For more information, download the brochure below.
POLYPS
For more information, download the brochures below.
ANAL FISSURE SURGERY
For more information, download the brochure below.
GENERAL INFORMATION
For more information, download the brochure below.
HIGH RESOLUTION ANOSCOPY
Who may be recommended to have a HRA?
HRAs are only performed on people in whom there is a concern that anal cancer may develop, and in people who are participating in clinical trials. It is only performed in a small number of centres around Australia.
Is any preparation required?
Your routine hygiene measures are all that is necessary. The anal canal does not contain any faecal material, unless you actively want to go to the toilet.
It is currently not clear whether you should avoid douching (washing the inside of the anus) on the day of the procedure. However, some specialists think that douching may wash away some of the cells that we are specifically looking for, so ask that you avoid doing this for 24 hours before you are seen.
What is involved in a HRA?
You will be booked in for a one hour appointment, although the procedure typically only takes around 15-30 minutes. It is performed in a specially equipped, private room.
We ask you to remove the lower half of your clothes and then give you a gown. Using lubricant mixed with local anaesthetic, a small tube (anoscope) is inserted into the anus and then special dyes (5% acetic acid and Lugol’s Iodine) are introduced. Sometimes some of the excess dye causes a sensation of wetness on the buttocks.
Dr De Lacavalerie will then look inside, using a high powered microscope (a “colposcope”). After careful, thorough examination of the area, you may be informed that there are some abnormalities present and that a biopsy may be indicated.
What is involved in an internal anal biopsy?
A biopsy is a small sample of tissue that is sent to the laboratory for analysis. It is removed from inside the anus using special tweezers. Most people undergoing internal anal biopsies do not feel anything, as there are few nerve endings present in this area. The specialist will let you know when this is about to happen. It is quite common for several biopsies to be taken.
What is involved in a perianal examination?
As part of the HRA assessment, the specialist will also carefully examine the outside edge of the anus (the perianal skin), following the application of a dye. If any abnormalities are seen, then a biopsy will be suggested. Local anaesthetic will be used for this, and frequently a stitch will be used, to promote rapid healing. Stitches are then generally removed 5-7 days later.
What happens after the HRA?
You will be given some pads to place in your underwear, as there is often slight bleeding for 24-48 hours after the procedure. Occasionally there is a further, slight bleed 4-5 days later, as the internal scabs fall off. Opening your bowels can often trigger slight bleeding, but it usually stops very quickly. It is recommended that you do not do anything strenuous (such as going to the gym or swimming) on the day of the procedure. For the following week, you are advised not to have receptive anal intercourse, or to use anal toys. Some people like to increase the fibre content of their diet to help make the stools softer.
If you are concerned about any symptoms developing after the procedure, contact the department for advice.
Healing of the biopsy sites occurs very quickly, usually without any scarring. All procedures are done using sterile or single-use equipment. Infections are very rare, as the lining of the anus has a very strong immune system.
Depending on what is found at the HRA, you may be asked to return in a couple of weeks for the results. At this point, the specialist will discuss any treatments or further follow up advised.
PRURITUS ANI
For more information, download the brochure below.
GENERAL INFORMATION
For more information, download the brochures below.
ROBOTIC SURGERY
Colorectal conditions
The lower part of your digestive tract, called the large intestine, is comprised of the colon and rectum and is also sometimes called the colorectal region. It can develop issues that range from occasionally bothersome to life-threatening. As an example, colorectal cancer is the third most common cancer in men and women who live in the U.S., with more than 145,000 new cases expected in 2019.1
There are also a number of noncancerous conditions that can cause pain and discomfort. These include, but are not limited to, inflammatory bowel diseases like Crohn’s disease and ulcerative colitis, blockages and ruptures, infected pockets (diverticulitis) and abscesses, and others that can take a toll of your quality of life and may require medical care. In the case of cancer or when lifestyle changes, medicine, and other options do not ease symptoms of noncancerous conditions, your doctor may suggest surgery.
Types of surgery
In the past, surgeons made large incisions in skin and muscle so that they could directly see and work on the area of concern. This is called open surgery. Today doctors still perform open surgery, but can also perform many colorectal procedures using minimally invasive laparoscopic or robotic-assisted surgery, possibly with da Vinci technology. Both minimally invasive surgical options require a few small incisions that doctors use to insert surgical equipment and a camera for viewing. In laparoscopic surgery, doctors use special long-handled tools to perform surgery while viewing magnified images from the laparoscope (camera) on a video screen.
What is a da Vinci surgical system?
Da Vinci surgical systems are comprised of three components: surgeon console, patient-side cart, and vision cart.
Surgeon console
The surgeon console is where your surgeon sits during the procedure, has a crystal-clear 3DHD view of your anatomy, and controls the instruments. The tiny instruments are “wristed” and move like a human hand, but with a far greater range of motion.
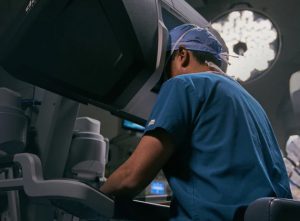
Patient cart
The patient-side cart is positioned near the patient on the operating table. It is where the instruments used during the operation move in real time in response to your surgeon’s hand movements at the surgeon console.
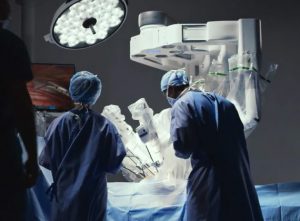
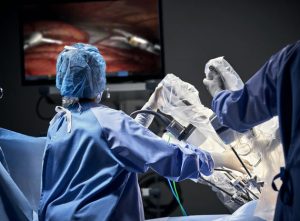
Vision cart
The vision cart makes communication between the components of the system possible and provides a screen for the care team to view the operation.
It’s important to remember that Intuitive does not provide medical advice. After discussing all options with your doctor, only you and your doctor can determine whether surgery with da Vinci technology is appropriate for your situation. You should always ask your surgeon about his or her training, experience, and patient outcomes.
1. Key Statistics for Colorectal Cancer. American Cancer Society. Web. 23 January 2019.
https://www.davincisurgery.com/procedures/colorectal-surgery
BOWEL ENDOMETRIOSIS
This leaflet covers endometriosis and the bowel. It provides information for those who have been diagnosed or are undergoing investigations for endometriosis on the bowel. Medical terms are in italics. If you have any questions Dr De Lacavalerie is happy to answer them for you.
What is bowel endometriosis?
Endometriosis can affect the bowel in the abdomen and pelvis. It can be on the surface of the bowel (superficial) or penetrate into the bowel wall (deep endometriosis). Bowel endometriosis or Recto-vaginal nodules probably start superficially on the surface and progress to deep infiltrating disease growing through the wall of the bowel. There are many theories, but the exact cause of endometriosis is not known.
What are the main symptoms of bowel endometriosis?
Symptoms of bowel endometriosis include pain on opening the bowels, described by some as “a bread-knife up the bottom” (dyschezia), and deep pelvic pain with sex (dyspareunia). Some people experience rectal bleeding during their period.
It is common people with bowel endometriosis to also be diagnosed with irritable bowel syndrome (IBS). Endometriosis and irritable bowel syndrome can occur together. The difference is that symptoms of bowel endometriosis vary throughout the menstrual cycle; they are worse in the days before and during a period. Try keeping a note of your symptoms to see if they vary at different times of the month.
How is bowel endometriosis diagnosed?
Dr De Lacavalerie will ask you questions about your symptoms and examine you. This may involve a vaginal examination, ultrasound scan, and a day case procedure to look inside the bowel with a small camera (flexible sigmoidoscopy), and/or a laparoscopy (a keyhole operation to look inside your pelvic area). CT scan and MRI may be helpful if you are thought to have deep endometriosis inside the bowel wall. It is not always possible to know how badly your bowel is affected by endometriosis until your operation.
What are the treatment options for bowel endometriosis?
Treatment options include doing nothing, medical or complementary therapies to manage symptoms, and surgery. The ‘do nothing’ option may be appropriate in your case if you have mild symptoms or no symptoms.
What are the medical treatments?
Medical treatments offered include painkillers (analgesics) and/or anti-inflammatory drugs. Opiate based painkillers such as codeine are constipating which can make bowel symptoms worse.
A key management strategy for endometriosis is centered on ‘tricking’ your body into thinking that you are pregnant by using hormones called progestagens or contraceptives (like the Pill or Mirena), or that you are menopausal (using medicines like danazol or those called gonadotrophin releasing hormone agonists). Current evidence suggests that there is no difference in terms of pain relief between either strategy – all approaches appear equally effective and may provide benefit for up to six months following the end of treatment.
What happens during surgery for bowel endometriosis?
The aim of surgery is generally to cut out (excise) all of the endometriosis. In the majority of cases, surgery can be carried out laparoscopically (keyhole), robotically or via open surgery (laparotomy), depending on the surgeon and your situation. Robotic and laparoscopic surgery may reduce adhesions and recovery time.
There may be two or more surgeons present depending on the extent of your endometriosis. Usually this will include a Colorectal Surgeon and a Gynaecologist with experience of this type of surgery, and in some cases, a Urologist or Urogynaecologist.
There are three main options for the bowel aspect of your surgery:
- The segment or section of the bowel containing the endometriosis can be The bowel is then re-joined (re-anastomosis).
- For smaller areas of endometriosis, a disc of the affected tissue can be cut away and the hole in the bowel closed.
- Alternatively, the endometriosis or nodule can be ‘shaved’ off the bowel leaving it intact. This option may leave residual endometriosis.
Surgery should be tailored to the individual and their symptoms and needs. Most people (approximately 75%) can have conservative surgery, preserving their fertility.
With any bowel surgery there is a possibility that a temporary colostomy will be needed. This is a procedure where a section of your bowel is attached to an artificial opening on the tummy wall. This opening is known as a stoma. A stoma bag stuck to the skin of your tummy collects faeces. If it is thought that you might need a stoma, we will arrange for you to talk to a specialist nurse, and you will have time to discuss this with Dr De Lacavalerie in advance.
This type of surgery is difficult and may take several hours. It also may not be possible to perform the operation by laparoscopy; in 1 in 7 cases, the operation is changed to a laparotomy (a procedure involving a bigger incision in your tummy to gain access to the bowel). Although this is rare when your surgery is performed in a multidisciplinary team like Womens Health Road offers.
About one in ten people have major complications;
- when the bowel is joined together the stitches may not heal properly resulting in a leak in the bowel. This may require a second emergency operation and you may need a temporary stoma while your bowel heals.
Most complications are not serious and include a high temperature, infection in the stitches, and a chest or urine infection, these can be treated with antibiotics. Antibiotics may also be given routinely to try and prevent infection. You will given TED stockings to wear try and prevent a venous thromboembolism (a deep vein blood clot) or pulmonary embolus (a blockage of an artery in the lungs). You may experience difficulty emptying your bladder after the operation, this is temporary and returns to normal with time and recovery.
What can I expect after my operation?
You can expect to feel sore. You will be given painkillers before you wake up and can have more in recovery until you are comfortable enough to go back to the ward. Your anaesthetist may discuss an epidural or patient controlled analgesia (PCA) with you. A PCA connects with the drip in your arm, and you have a button to press which delivers a set amount of painkiller. You can start drinking water immediately after your operation and build up to eating. If you feel sick or do vomit after the operation the nurses will give you anti-nausea medication to help reduce this.
In some cases, you may be transferred to a high dependency unit (HDU) for a short time – this means that you can be monitored more closely.
It is not uncommon for your bowels not to work for up to seven days after the operation. You may be prescribed a gentle laxative to help get your bowels moving. Drinking plenty of water also helps. You should avoid straining to go to the toilet. You will not need to stay in hospital until you open your bowels, as long as you are passing wind consistently.
When can I go home from the hospital? When will I feel back to normal?
Recovery time, both in hospital and at home, varies from one person to another. Don’t try and compare yourself to how others are recovering. After laparoscopic bowel surgery, you can usually go home after 1–3 days, and if the operation is performed via a laparotomy (open surgery) after 5–7 days.
By the time you go home you will be able to get up and move about. You may need to take regular painkillers for the first few weeks. You can gradually return to normal daily activities. A gentle walk every day is beneficial; try and do a little bit more every day, but stop if you feel pain. You can go back to driving when you have stopped taking strong painkillers (which might make you drowsy), and can comfortably sit in the car seat and turn to look in the mirror and do an emergency stop.
How much time you will need to be off work depends on the type of work that you do. You can expect to be off work for at least 10–14 weeks after major bowel surgery. It may take six months before you feel fully back to normal.
Bowel function may be altered following this type of surgery, particularly with a full resection (re-anastomosis). This does improve over time although some people may need to watch their diet to see which foods aggravate or improve symptoms. Some patients may benefit from the advice and support of a nutritionist. It is important to discuss any concerns with Dr De Lacavalerie.
After going home, you should contact your GP, Dr De Lacavelerie or your nearest emergency department if you have any of the following:
- Swelling or redness of any wound
- Bleeding, discharge or a foul smell from any wound
- Nausea, vomiting or loss of appetite
- A high temperature (more than 38oC)
- Not passed flatus (wind from your bottom or your stoma if you have one) for more than 48 hours and have abdominal pain
- Abdominal pain that is getting worse.
Does bowel endometriosis have to be treated? What are the risks of not having treatment?
Whether or not bowel endometriosis requires treatment depends on your case, your symptoms and how severe the endometriosis is. Dr De Lacavalerie is here to help you and explain your treatment choices. The final decision is yours.
Without treatment or management, your symptoms are likely to continue and may get worse over time. Endometriosis is a progressive disease and gets worse in about 50% of people, this can lead to that deeply infiltrating endometriosis that penetrates through to the inside of the bowel.
RECTAL PROLAPSE SURGERY
For more information, download the brochures below.
TRANS-ANAL RECTOCELE REPAIR (STAMP PROCEDURE)
This page provides information about surgery to repair a rectocele. This information is intended only for patients under the care of the Shrewsbury and Telford Hospital Pelvic Floor Service. It may not cover everything you want to know so please ask if you need further information.
What is a rectocele?
A rectocele is a bulge or weakness at the front of your rectum which can cause difficulty with emptying your bowels. You may not feel empty after evacuation, needing to help the stools out with your fingers or experience leakage afterwards.
Why is this operation performed?
The operation corrects the bulge in your rectum so that bowel evacuation is more normal. It is done this way either when it is either not possible or not necessary to perform an operation through your abdomen. Your Consultant will discuss this with you further.
What does the operation involve?
The operation is performed under a general anaesthetic and takes around 1 hour. All the surgery is done through your bottom (back passage) so there are no external sutures or wounds. You may be given an enema before the operation to ensure your lower bowel is empty. The baggy inner lining (mucosa) is separated from the underlying muscle layer of the rectum. Any excess mucosa is trimmed. Dissolvable stitches are placed in the thinned and floppy muscle layer to repair the rectocele and strengthen the muscles. The lining (mucosa) is then re-stitched to cover the underlying muscle repair.
What is the recovery like?
Immediately after the operation you will normally have a urinary catheter in place (a tube into your bladder) and a drip in your arm. You will be prescribed a course of antibiotics for 7-10 days. You may eat and drink as soon as you want to after the operation. The drip will be removed once you are drinking enough. Simple painkiller tablets will usually be enough to keep you comfortable following the operation.
Your catheter will generally be removed in the evening on the same day as your operation and you should be able to go home when you are comfortable and passing urine normally, this is usually the next day. You will go home on a course of laxatives (usually macrogol or movicol) for 6 weeks so do not strain to evacuate. You can gradually reduce the laxative if your bowels are too loose but don’t allow yourself to get constipated, especially in the first few weeks after surgery, as this may damage the repair.
Keep mobile after your surgery but avoid heavy lifting (anything heavier than a full kettle), sexual intercourse or strenuous exercise (running, jumping, squats etc.) for 6 weeks as this may cause excess strain on the pelvic floor muscles. Avoid activities such as shopping, housework, lifting children and sports as these can delay healing. You can shower and bathe as normal after the operation. You should be fit to drive after about 1 or 2 weeks and return to work after 2 to 4 weeks.
Outcome of surgery
Surgery results in a good improvement in symptoms of around 8 out of 10 patients but additional nonsurgical treatments can help with the symptoms. There is around a 6 to 7% risk of recurrence following the operation. It will usually take several months for your bowels to settle down into a regular pattern after surgery. Less than 5% of patients report worsening of symptoms after this surgery.
What are the risks?
You will have the opportunity to discuss all the risks and benefits of the operation with Dr De Lacavalerie before signing the consent form. As the surgery is performed through your bottom there is a risk of weakening your bowel control. The risk is greater if you already have bowel control problems. To minimise this risk we assess the strength of your anal sphincter muscles first. If you do not wish to risk worsening bowel control alternative non-surgical options will be discussed with you.
There is a small risk of bleeding after surgery and you may notice minor blood spotting when passing stools. You may also experience minor bleeding 4 to 8 weeks after the operation when the stitches start to dissolve. A wound infection can occur following surgery. Infection may cause discomfort and can result in a discharge through the back passage which can delay healing. This may require further antibiotics; it can delay your discharge from hospital, and in a few cases may require further surgery.
Follow up
You will receive an appointment to be seen in Dr De Lacavalerie’s rooms around 2 to 4 weeks after your surgery. Further outpatient appointments will be arranged as necessary.
GENERAL INFORMATION
For more information, download the brochure below.
CROHN'S DISEASE
For more information, download the brochure below.
ULCERATIVE COLITIS
For more information, download the brochure below.